Meet Ava. AI intelligence for benefits teams.
Design smarter programs and improve benefits ROI—with AI agents that monitor your entire program, surface what matters, and give you insight into costs and outcomes in seconds.

“Benefits are managed from the rearview mirror. Ava lets us see what’s in front of us for the first time.”
Director of Benefits, Manufacturing Company
Get a complete and objective view of your benefits program with all your data in one place
Take control of benefits spend with cost-saving insights — surfaced before you need to ask
Go from fighting fires to managing benefits proactively with ongoing intelligence
How it works
01
Train Ava on your benefits
Ingest contracts, SPDs, carrier agreements, and policy documents. Build a complete understanding of your plan designs and coverage rules.
02
Connect other data sources
Integrate with carriers, TPAs, and HRIS to analyze real-time claims, utilization trends, and workforce demographics.
03
Start getting insights instantly
Ava proactively surfaces what needs attention and answers questions in natural language — no dashboards to build or queries to write.
Dozens
of data feeds, documents, and systems unified per customer
Millions
of dollars of claims analyzed per customer
42 seconds
average time to answer strategic questions on ROI, costs, or outcomes
"Avante isn’t just decision support, advocacy and care navigation. Or data warehousing. Avante provides everything, and that's what's been missing in the market."
Tyler Ingram
SVP, Health & Benefits
.svg)

SOC 2 Type II Certified
Enterprise-grade security
GDPR compliant
HIPAA compliant
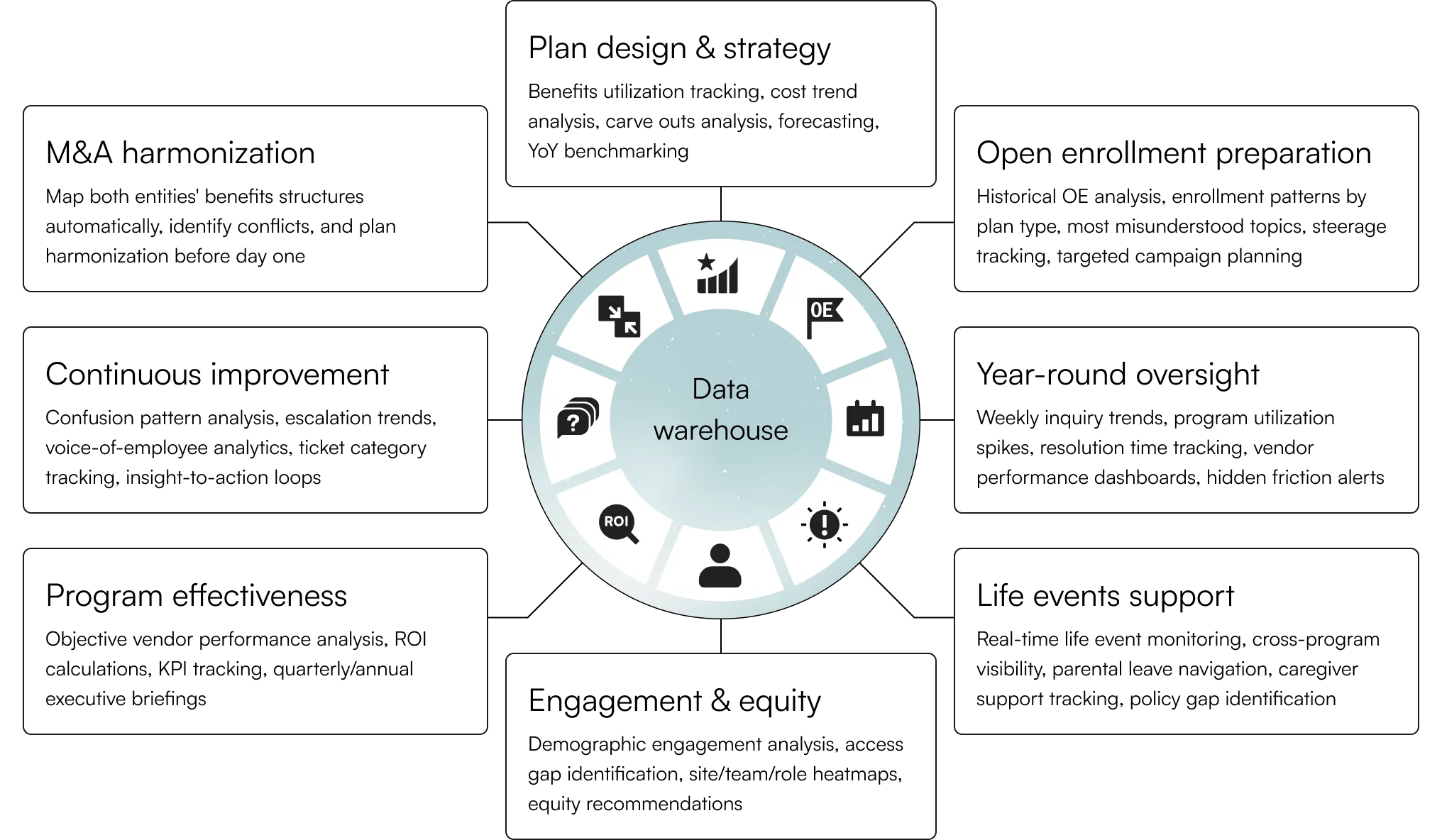
Analyses from planning to performance
Plan design & strategy
Benefits utilization tracking, cost trend analysis, carve outs analysis, forecasting, YoY benchmarking
Open enrollment preparation
Historical OE analysis, enrollment patterns by plan type, most misunderstood topics, steerage tracking, targeted campaign planning
Year-round oversight
Weekly inquiry trends, program utilization spikes, resolution time tracking, vendor performance dashboards, hidden friction alerts
Life events support
Real-time life event monitoring, cross-program visibility, parental leave navigation, caregiver support tracking, policy gap identification
Engagement & equity
Demographic engagement analysis, access gap identification, site/team/role heatmaps, equity recommendations
Program effectiveness
Objective vendor performance analysis, ROI calculations, KPI tracking, quarterly/annual executive briefings
Continuous improvement
Confusion pattern analysis, escalation trends, voice-of-employee analytics, ticket category tracking, insight-to-action loops
M&A harmonization
Map both entities' benefits structures automatically, identify conflicts, and plan harmonization before day one
Consolidate all your data in one place
Secure repository
Ingest SPDs, contracts, claims feeds, vendor agreements, HRIS data, and conversation patterns into one searchable platform
Institutional memory
Complete history of plan decisions, vendor negotiations, and benefits philosophy. Never lose context when teams or clients transition
Clear organization
Documents organized by plan, vendor, and topic. Ava knows which contracts apply to which populations and what data sources to query for each question type.
Get strategic insights before you need to ask
Opportunistic insights
Ava surfaces patterns and anomalies you didn't think to ask about — before they become problems.
Recurring analyses
Schedule analyses to refresh automatically, so critical insights stay current.
Shared intelligence
Share custom analyses with the Avante customer community, learning from peers how they're optimizing benefits.
Produce analyst-grade reports in minutes
On-demand analysis
"What's our fertility program ROI?" "Are GLP-1s improving health outcomes?" "Which vendors are underperforming their SLAs?" Ask any question and get comprehensive, cited answers.
Expert-level depth
Go deeper with follow-up questions and modeling: "What if we switched to a different carrier?" "How would a 10% premium increase affect enrollment?" "Show me the cost breakdown by age cohort."
Connect systems. Unlock intelligence.
01
Documents
Upload SPDs, carrier contracts, vendor agreements, and benefits guides. Ava audits for conflicts and delivers immediate value from contract search and policy Q&A.
02
HRIS
Connect read-only API to Workday, ADP, or UKG. Unlock eligibility analysis, population insights, and demographic trends for strategic planning.
03
Claims & vendor feeds
Establish secure carrier and vendor API connections as available. Unlock cost trend monitoring, utilization tracking, and vendor performance evaluation.


.svg)
.svg)
.svg)











